Palpitations
Indice dell'articolo
WHAT ARE PALPITATIONS?
Palpitations are a disorder, characterized by the perception of the heartbeat, which may be due to the acceleration or irregularity of the heart rhythm.
In fact, there is talk of palpitation both in the case of a physiological (or normal) increase in heart rate (also called “sinus tachycardia”), which can be induced by physical effort and emotion, and in the event of irregular heart rhythm, called “arrhythmias”.
The arrhythmias causing palpitations can be of various origins, both supraventricular (or atrial), and ventricular, and can be isolated, called “extrasystoles” (felt as a “failure to beat”) or, if prolonged, due to supraventricular paroxysmal tachycardias or atrial fibrillation, or in rare more severe cases, ventricular tachycardias.
WHAT ARE THE CAUSES OF PALPITATIONS?
The causes of palpitations can be of a nervous nature (anxiety, stress), or be due to intoxications (in particular inhalation of fumes or carbon monoxide), or to non-cardiac disorders (in particular gastro-esophageal, pulmonary, allergic crisis, anemia or thyroid diseases), or to cardiac causes, in particular ischemic heart disease, ventricular hypertrophy, heart failure, heart valve disease, and electrical heart disease.
The clinical features that suggest a cardiac origin of palpitations are as follows:
- Presence of anomalies of the ECG trace
- Known organic heart disease (ischemic heart disease, myocardial hypertrophy, valvulopathies, heart failure)
- Known electrical heart disease (e.g. Wolff-parkinson-White syndrome, Brugada syndrome, Long QT syndrome)
- History of previous arrhythmias (e.g. paroxysmal atrial fibrillation)
- Family history of sudden death
- Old age (or very young)
Palpitations can be associated with real pain in the thoracic site (precordialgia or angina) and in this case they direct the diagnosis towards problems related to the presence of cardiac ischemia (i.e. a spraying defect of the heart muscle due to the presence of stenosis (or narrowing ) of the heart arteries (called coronaries).
Palpitations can precede an episode of syncope (or loss of consciousness) and also in this case it is important to report it, as this symptom directs the diagnosis of the syncopal episode as being due to the presence of cardiac arrhythmias.
HOW IS DIAGNOSIS CARRIED OUT WHEN THERE ARE PALPITATIONS?
The first choice examination for the diagnosis of palpitations is the Holter dynamic ECG, preferably not only 24 hours, but prolonged, that is, recording the ECG trace for the duration of at least 7 days up to a maximum of 30 days, depending on the frequency of symptoms.
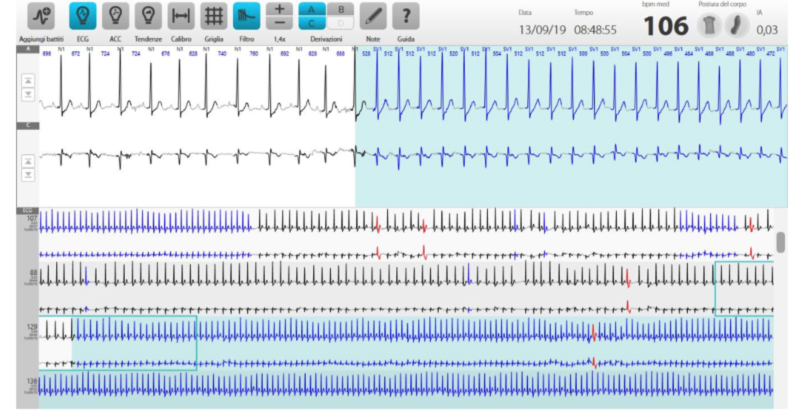
Example of paroxysmal supraventricular tachycardia recorded during prolonged Holter during palpitations
Furthermore, systems for recording short traces in conjunction with symptoms have also recently been proposed, directly via smartphone or i-watch, which also allow you to send the track directly to your doctor (system called “cardiotelephone”).
Then there are recording systems that are implanted subcutaneously that allow the recording of the heart rhythm up to 2-3 years, and regularly send the tracks through the remote monitoring system.
Again, another test often used in case of palpitations is the stress test, to verify the onset of any heart rhythm disturbances during exercise. In some cases, an electrophysiological study or a provocative study with drugs (ajmaline or isoproterenol) may be needed to complete the diagnosis.
It will be the duty of the arrhythmologist in case of palpitations to choose the most suitable system according to the case to make the diagnosis of the heart rhythm disorder, and then monitor over time the effectiveness of the different treatments (antiarrhythmic drugs or transcatheter ablation).
In addition to recording the heart rhythm, different morphological tests (echocardiogram, cardiac magnetic resonance, coronary angio-CT, or coronary angiography) are also necessary, to establish the presence of any cardiac or coronary artery disease.
WHAT TO DO IN CASE OF PALPITATIONS?
In case of palpitations, both in case of tachycardia and extrasystoles, it is good to stop any activity in which you are involved and try to relax to return the heartbeats to normal. A good practice is to lie down whenever possible and try to breathe deeply.
In the event that palpitations lasts for a long time (over an hour) or are associated with a feeling of fainting, or it is believed that there is a risk of anaphylactic shock, carbon intoxication, or pulmonary or cardiovascular diseases (see list of associated diseases) it is good to contact the Emergency Department. In other cases, consult your doctor as soon as possible.
Bibliography
Locati ET. New directions for ambulatory monitoring following 2017 HRS-ISHNE expert consensus. J Electrocardiol. 2017 Nov – Dec;50(6):828-832. doi: 10.1016/j.jelectrocard.2017.08.009. Epub 2017 Aug 12. PubMed PMID: 28928046.
Locati ET, Moya A, Oliveira M, Tanner H, Willems R, Lunati M, Brignole M. External prolonged electrocardiogram monitoring in unexplained syncope and palpitations: results of the SYNARR-Flash study. Europace. 2016 Aug;18(8):1265-72. doi: 10.1093/europace/euv311. Epub 2015 Oct 29. PubMed PMID: 26519025; PubMed Central PMCID: PMC4974630.
Rosano GM, Rillo M, Leonardo F, Pappone C, Chierchia SL. Palpitations: what is the mechanism, and when should we treat them? Int J Fertil Womens Med. 1997 Mar-Apr;42(2):94-100.
